Fibromyalgia Information & Local Support
Honours for this website
Fibromyalgia Information & Local SupportHonours for this website |
 |
Written by David A. Nye MD
Syndromes are certain constellations of symptoms and signs or lab findings. They are different from diseases which are defined by their causes. Anyone who has the symptoms and exam findings that define a syndrome has that syndrome by definition, whatever the underlying disease mechanism. Two different diseases may cause the same syndrome. Two different syndromes may be caused by the same disease.
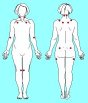
A diagnosis of fibromyalgia syndrome requires a complaint of aching all over and the finding of at least 11 out of 18 tender points on examination. A diagnosis of chronic fatigue syndrome requires that other criteria be met, including disabling fatigue and the presence of a certain number of other signs and symptoms, several of which are also common to FMS.
Although CFS and FMS are differently defined syndromes, it is likely that patients with fibromyalgia and chronic fatigue syndromes have the same underlying disease. The majority of patients who meet the criteria for one do so for the other. It seems unlikely that patients meeting the diagnostic criteria for both have two separate diseases.
Symptoms are similar in the two disorders. Effective treatments for one often turn out to be effective for the other. Most CFS experts now acknowledge the value of gentle aerobic exercise in treating CFS, although in both disorders, too much or too vigorous exercise is harmful. Similar laboratory abnormalities are being uncovered in both.
This has led to the suggestion that the distinction between the two is artificial and exists largely for historical and territorial reasons. Perhaps dividing the two disorders depending on the degree of fatigue relative to pain is no less arbitrary than dividing these patients into two groups depending on whether or not they have dizziness, tingling, pelvic pain, or any of the other dozen or more symptoms associated with these disorders.
This is not just a semantic "lumper vs. splitter" debate. If FMS and CFS are produced by the same underlying disease process, we are wasting research money and effort and slowing progress toward discovering the pathophysiology by not combining CFS and FMS research efforts, not to mention confusing patients and the public.
The prevalence of FMS is 2-4%, well above the estimated prevalence for CFS. If the two conditions are indeed caused by the same disease, that means that FMS is a more sensitive index for it. It has been estimated that at least 75% of FMS patients become at least 75% better with treatment. In my experience this is somewhat low given recent advances n treatment. The higher reported success of treatment of FMS than CFS suggests it might also be more specific, or at least does not acheive it's sensitivity at the expense of reduced specificity.
A diagnosis of FMS does not require the extensive and expensive workup that CFS does, which requires that other causes of fatigue be excluded. In fact, there is no recommended routine minimum diagnostic evaluation for FMS. Whether this is because the presence of tender points is highly specific for this disease or because the recommended workup is not really necessary merits further study. I have had no FMS patients who turned out later to have a different problem masquerading as FMS and one doesn't read about this being a problem in the literature.
These considerations suggest that we should use the diagnosis of CFS only in patients who fail to meet diagnostic criteria for FMS, or better yet allow the diagnosis of a new combined syndrome in some patients who fail the tender point criteria if they meet other symptomatic criteria CFS currently associated with CFS.