Fibromyalgia Information & Local Support
Honours for this website
Fibromyalgia Information & Local SupportHonours for this website |
 |
©Devin Starlanyl, MD 1995-1998 & Ken Hoelscher
You have seen patients with fibromyalgia and myofascial pain syndrome, and will see more. They are both very real medical conditions, and both very different, although often confused. They may be the answer to some of your "challenging" patients. Although the conditions may seem like a diagnostic nightmare to you, try to imagine what your patients have been dealing with.
Fibromyalgia is a systemic neurotransmitter condition with, among other things, a disrupted adrenal-hypothalamus-pituitary axis. It is nonprogressive (although it may seem so), nondegenerative, and noninflammatory. It is responsible for diffuse body-wide pain, tender points that hurt but don't refer pain, and sleep disturbances. It is NOT a "wastebasket" diagnosis.
Chronic myofascial pain syndrome (MPS) is a musculoskeletal chronic pain syndrome. It is nonprogressive (although it may seem so), nondegenerative and noninflammatory. It is composed of many Trigger Points (TrPs), which refer pain and other symptoms in very precise, specific patterns. It seems progressive because each TrP can develop satellite and secondary TrPs, which can form secondaries and satellites of their own. With treatment of the TrPs and underlying perpetuating factors, however, these TrPs can be " reversed" and minimized or eliminated. It is NOT a "wastebasket" diagnosis.
When occurring together, what I call the "FMS&MPS Complex Complex" forms. This is a condition of interconnected symptom spirals that get increasingly worse until the spiral is interrupted. For example, pain causes muscle contraction which causes more pain which causes more contraction, etc. The patient can sometimes have muscles that are like cement, due to myofascial splinting.
Any patient with diffuse body-wide aches of long duration, coupled with a sleeping disorder -- inability to fall asleep, inability to stay asleep, light sleep, inability to get restorative sleep, and/or waking early should be evaluated for FMS. Those sleep problems indicate the alpha-delta sleep anomaly so common in FMS. Patients with specific patterns of referred pain (trigger points), indication of blood vessel, lymph or nerve entrapment or proprioceptive disturbances should be evaluated for myofascial pain syndrome.
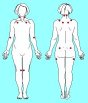
Tender points of FMS hurt in place, and are often found in the specified "18 locations". In cases of traumatic FMS, they may be clustered near trauma sites (including degenerative changes or surgical incisions). Muhammad Yunus, M.D. has found that a good indicator of proper pressure to test for tender points of fibromyalgia is when using the thumb to press you notice a blanching of the fingernail. That gives 4 kg pressure.
Trigger Points of chronic MPS refer pain. They may be active or latent. Latent TrPs restrict movement, but don't cause pain until they are activated by immobility, stress, or one of many possible perpetuating factors (see Symptoms).
Pain is a large factor in FMS and MPS. The general diffuse aching of FMS should not be confused with the specific sites and other symptomology of MPS.
Your patient may be confused or stressed during an office visit. S/he may have gone through misdiagnosis and may have taken a lot of blame. On the Internet, we call it the "It's All In Your Head" syndrome, or IAIYH. Ask a family member to come with them.
If relevant, order tests like the anti-candida antibody* and B2T panel to eliminate co-existing conditions which might be contributing factors. Look for indications of reactive hypoglycemia. It is very common in FMS&MPS Complex. You could use the Diagnostic Consult available elsewhere on this web site. Take the time to talk with your patient. Take the time to LISTEN. If you ask the right questions, you'll find out what you need to know. Take a GOOD history.
IT IS NOT UNUSUAL IN CASES OF FMS&MPS Complex COMPLEX FOR THE MUSCLES TO FEEL LIKE CEMENT. YOU OFTEN WILL NOT BE ABLE TO PALPATE THE TRIGGER POINTS OR TENDER POINTS. Sometimes altered HPA axis, altered metabolism and reactive hypoglycemia have conspired to create an obesity which is refractive to any attempts the patient has made to lose weight.
Overweight and/or extreme muscle guarding can occur in FMS or MPS alone. In this case, rely on your history. Once galvanic muscle stimulation, "spray and stretch" and other physical therapy modalities are used to break up the myofascial splinting, and the perpetuating factors are brought under control, you will be able to palpate the points.
Janet Travell speaks of "The Mystery of History". A careful history is the most important part of the physical exam. Dig for perpetuating factors, such as short upper arms. They are listed in detail in the Trigger Point Manual, as well as means to prevent their recurrence. Some muscles, like the deltoid, refer pain only locally. Some, like the scaleni, refer pain and other symptoms extensively. Check out "Myofascia Pain and Disfunction: The Trigger Point Manuals Volume I and II", by Travell and Simons (TPMs). The causes, perpetuators and remedies for trigger points are there.
Turn your patient's head to the side, and you may be able to feel ropy bands along the sternocleidomastoid (SCM) and the back of the neck. It takes practice. The SCM sets off referred pain in head and face, transmits faulty proprioceptor nerve impulses that inform the brain of the position of the head and body in the surrounding space. In cases of FMS&MPS Complex Complex, it lies. Eye problems, sometimes caused by eye muscle TrPs leading to irregular constriction and muscle imbalances cause the eyes to tell lies to the brain also, but different lies than the SCM. This can give your patient a drunken walk, as they bump into walls and door jambs. If your patient has long-standing TrPs in four quadrants with spinal involvement, your patient has MPS.
Growth hormone has a powerful effect on the connective tissue. It directly stimulates the production of fibroblasts and mast cells, ground substance and collagen fibers. It's significant in wound healing, where rapid production of collagen fibers by many fibroblasts is necessary for repair. But growth hormone is released during delta-level sleep. People with FMS usually have the alpha-delta sleep anomaly. The patient with fibromyalgia never enjoys delta level sleep, and suffers from chronic sleep deprivation. When delta sleep is reached, alpha waves intrude and jolt your patient back to shallow sleep or wide awake. It is vitally important that your patient gets restorative sleep, not just enough hours. FMS patients have very low levels of growth hormone. The body can't repair itself. Connective tissue is the major repair mechanism of body. Its chemistry monitors inflammatory response, and its fluids deliver antibodies and wbc to fight infection. All of these are disrupted in FMS. Immune killer cells are present in the normal amounts, but most are dormant.
It's not uncommon for your patient to feel nausea or a dramatic increase in muscle aches, especially headaches, and/or exhaustion after any bodywork has moved a large amount of toxins and wastes from constricted muscles. Exercise that doesn't place a lot of pressure on joints and helps muscles stretch is best. The usual limit is 5 to 8 minutes a day at first. Range of motion exercise is helpful. We tend to push ourselves, and when we do, the reaction is often delayed -- sometimes for days.
High velocity chiropractic techniques trigger rebound pain, especially with rotation of the neck. When there is nerve entrapment, the pain caused by this can be severe. Most people do tolerate Activator adjustment, strain/counterstrain and myofascial and CranioSacral release.
Some people blame FMS on deconditioning. This has been shown to be a fallacy. Everyone who is deconditioned physically will not get FMS. Some people who are extremely athletic develop FMS as a result of trauma received when they are still in peak condition.
Patients with FMS have an increased sensitivity to their own fight or flight neurotransmitters (catecholamines). They get caught in a neverending stress response that won't let them go (see Definitions).
The most common perpetuating factors of trigger points (TrPs) are fibromyalgia, impaired sleep, reactive hypoglycemia, hypothyroid, inappropriate physical therapy, skeletal asymmetry and disproportion. Also to be considered are nutritional inadequacies, anything that impairs muscle metabolism, chronic infections, psychological factors, allergy, etc.
When your patient is experiencing rest pain for a considerable part of the time, the TrPs are very active. Physical therapy may need to be limited to gentle passive stretch and hot packs. At first, the patient may only be able to tolerate a short session once a week. This is due to the releasing toxins, which must be processed by the liver and kidneys. See my video for ideas on how to stage the illness, and how to set up a treatment regimen. I have seen many people who were put into weight training and work hardening programs. This usually takes injured people and turns them into totally disabled ones.
A swimmer may drown from a muscle cramp produced by FMS&MPS Complex. Water temperature is critical to an FMS&MPS Complex patient, and should not vary from the 88 to 94 degree range. Undiagnosed FMS&MPS Complex pain has driven many patients to suicide. This pain can be all-consuming, and yet the patient looks fine. Because of their appearance, they are often denied the support that other handicapped patients take for granted. These conditions are neither controversial, nor are they to be dismissed lightly.
Suppose you lost the ability to practice medicine. You couldn't trust your fine motor control. Your hands often didn't work. Your ankles buckled. You couldn't get the right words out. Pain became a constant companion. You got lost on the way to the hospital, and it's only four blocks away. How would you feel? Depressed? Misunderstood? Congratulations. You'd be certifiable if you didn't feel overwhelmed and at least a little bit down. There is a relinquishment exercise in my book that can help you understand the constant strain of loss that people with FMS&MPS Complex face every day.
Acute pain that diminishes in the course of natural healing process is generally manageable psychologically. Recurrent or persistent pain due to an unrecognized cause threatens future function and well-being, which often leads to frustration, depression and progressive disability. When patients mistakenly believe that they must live with undiagnosed TrP pain because they are told it is due to arthritis, etc., they restrict activity in order to avoid pain. The TrPs become latent. Then must learn that TrPs are responsive to proper treatment.
People of any age can get FMS&MPS Complex, even pre-teens. Infant colic is often due to TrPs that can be relieved with gentle "spray and stretch" and CranioSacral Release. FMS in youth usually starts with a flu-like illness, and then manifests as "growing pains". If you catch it early, and teach your patient what is going on and how to handle it, you can give the young person with developing FMS&MPS Complex a good chance at life. Undiagnosed, children with developing FMS&MPS Complex are often shuttled aside as "behavior problems". Once you find the right combination of medications, physical therapy, and coping skills, your patient can avoid many of the absences from school that would otherwise occur. I have a chapter on FMS&MPS Complex in young people in my book, and have noted common childhood TrPs in my video, as they are likewise noted in the TPMs.
Visits with your patient should be about empowerment, not invalidation. Your patient may have gone through a traumatizing period of not being believed, meanwhile being racked by chronic pain of unknown origin. The patient must be encouraged to be an active manager and coordinator of the treatment team, and take responsibility for his/her own actions and consequences. Methods for accomplishing this are given in my book. Most patients had a high level of activity before FMS&MPS Complex became full-blown. Now they must be careful not to push it, and understand their limits.
If you get a chance to attend a seminar on FMS and/or MPS, do so. It will be worth your time. (A week or two devoted to the study of the Trigger Point Manuals would be well-worth it as well.)
Contact Robert Gerwin M.D or Walter Valliere M.D. at (301) 656-0220 for information on myofascial pain seminars.
Contact Mary Maloney P.T. for information on TrP hands-on treatment seminars at (203) 723-0533
Contact Richard van Why, R.N., M.Div., M.L.S. for information on fibromyalgia regional seminars at (301) 698-0932
Richard van Why gives this check list at his seminars, as a way to deal with trigger and tender points:
The "Journal of Musculoskeletal Pain" is an excellent source of new information, but don't neglect the Fibromyalgia Network Newsletter. It is a quick read, and summarizes much of the current research on-going. It also provides you with a birds-eye view of FMS, with hints on coping mechanisms.
The treatment of FMS&MPS Complex can be a "take up your bed and walk" kind of experience that is all too rare in a physician's life. It isn't unusual to see an undiagnosed patient come in on crutches, or even in a wheelchair, and have them walking within a few months. There is so much that you can do, and so much that they can do. The amount of study may seem overwhelming at first, especially when you look at the TPMs. Take it in short pieces, and it will reward you -- and your patients. The hard work has been done by Travell and Simons, and the answers are there. Keep the manuals on your desk and refer to them often. Think of them as an investment.Nowhere else could you get such a return on your time and money.
Test Information
* Anti-candida antibody test, Immunodiagnostic Laboratory, POB 5755, San
Leandro CA 94577 (800) 888-1113
IgG levels indicate a chronic problem. IgA reading indicates problems in mucous
lining of sinus, lung, gut, vagina. IgM reading indicates recent yeast problem.
**Total T4 and T3 uptake often gives false negatives for thyroid. We need B2T panel -- Total T4, Free T4, total T3 and TSH to indicate true state of thyroid. Patients with low-nromal thyroid often respond well to T3 therapy.